
My 5 Favorite Medicinal Herbs for Defeating Lyme Disease and Co-Infections
Lyme disease is the top vector-borne disease in the United States. The Centers for Disease Control and Prevention (CDC) estimates that around 300,000 Americans are diagnosed with Lyme disease each year. However, some research organizations believe that this number is much higher, in the range of 400,000. The disease is now found in all 50 states.
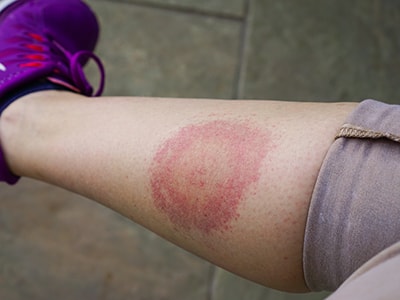
Symptoms of Infection
Symptoms begin with flu-like body aches, chills, neck and joint pain, sweating, headache, and fatigue. If left undiagnosed or if early antibiotic treatment is ineffective, the disease progresses into a chronic inflammatory response that mimics an autoimmune disorder, which can lead to:
- Insomnia and poor sleep
- Digestive complaints including nausea
- Severe joint pain and inflammation
- Chronic fatigue and lethargy
- Mood disorders such as anxiety and depression
- Cognitive issues that include brain fog, forgetfulness, headaches, and poor concentration
- Migraine headaches
- Heart or breathing problems
- Extreme sensitivity to light and sound
- Post Lyme Disease Syndrome (PLDS)
It is important to note that when Lyme disease remains persistent after early antibiotic intervention, it often indicates an underlying issue, including: weakened immunity, a wide-spread bacterial infection, mold exposure, or parasites. Post Lyme Disease Syndrome (PLDS) is when the initial Borrelia burgdorferi infection becomes chronic and causes continuing symptoms for many months or even years. These are the instances where antibiotic treatment has failed or the infection was left untreated. When this happens, it leads to a significantly lower quality of life for the patient. Ideally, prevention is key. But if you have developed Lyme disease and the antibiotic protocol was unsuccessful, several medicinal herbs are available that can help you heal.
My Top Herbal Recommendations for Healing
Reishi Mushroom
Antibacterial, anti-fungal, and anti-inflammatory, reishi is an excellent medicinal herb for treating Lyme disease. It also soothes the anxiety and depression that often accompany the disease. What’s more, reishi tackles arthritis, lupus, MS, heart disease, and cancer. Before using, make sure the tincture is dual-extracted and uses only the fruiting body, like the one found in my Apothecary.
Japanese Knotweed and Chinese Skullcap
This study found that Japanese knotweed and Chinese skullcap are more effective against B. burgdorferi in both the growing and non-growing stationary stage of the bacteria than the antibiotics doxycycline and cefuroxime. Japanese knotweed is also high in the bioactive compound resveratrol, which is a potent antioxidant and anti-inflammatory that assists in treating Lyme disease. Chinese skullcap is anti-inflammatory, neuroprotective, antioxidant, and also contains melatonin which is helpful for supporting restful sleep. It is known to treat bartonella and babesia co-infections as well.
Japanese knotweed and Chinese skullcap are included in my Eastern Blend Tincture, along with Japanese honeysuckle, and cordyceps mushroom. Not only is this tincture outstanding for fighting Lyme disease, but it is also helpful for insomnia, digestive disorders, respiratory issues, depression, fungal and bacterial infections, as well as colds, influenza, and other viral infections.
Wild Teasel
As a preventative and therapeutic herb, wild teasel is outstanding for treating B. burgdorferi infections. As I wrote in Struggling with Lyme disease? Wild Teasel may help:
“While teasel isn’t an antibiotic, it acts as a powerful agent to flush the bacteria into the bloodstream so that antibiotics can more easily target the infection. When dealing with Chronic Lyme Disease or in situations where the antibiotic protocol wasn’t effective, adding teasel into your treatment regime can make a tremendous difference. However, it may still take up to six months or longer to clear the infection.”
Cryptolepis
Found to be more effective than antibiotics against B. burgdorferi, this study established that a 1% cryptolepis extract caused complete eradication of the spirochete in vivo. Moreover, recent research published in Infectious Microbes & Diseases discovered that it also treats bartonella, a common Lyme co-infection that can cause mood swings, blurred vision, neurological impairment, brain fog, fatigue, anemia, and immune dysfunction. Bartonella is not only spread by ticks, but also fleas, lice and mosquitoes.
One of the most frustrating symptoms of Lyme disease is brain fog. If you are struggling with poor cognitive function, my Brain Bundle can help as it contains several brain-boosting botanicals, including: Lemon Balm, Lion’s Mane, Cordyceps, and Reishi.
Diet, Lifestyle, and Underlying Conditions
Lyme disease has many similar symptoms as autoimmune disorders like multiple sclerosis. So, it makes sense that many of the same helpful diet and lifestyle choices for MS also apply to Lyme disease. An organic, anti-inflammatory diet is crucial. As is managing stress and practicing gratitude.
Lastly, it is important that you address any underlying conditions that could hinder your healing, such as mold exposure, parasites, or sensitivity to Electromagnetic Fields (EMFs).









Where does goldenseal rank against these maladies?
Hi Bruce,
According to studies, these are the best herbs for Lyme disease and co-infections: Cryptolepis, Black walnut, Japanese knotweed, Sweet wormwood, Cat’s claw, Cistus incanus, Chinese skullcap.
Many blessings and good health!
Ledum (1M) appears to be the go to for Lyme with many Holistic Vets. It’s what I use as per my personal Vets recommendation and another I’ve consulted with via zoom due to being in different countryies.
Lately I’ve come across research and Herbalists recommending Teasel root as effective in fighting Lyme. I’ve no experience with it & I’m also just a lay person frequently searching because I have a dog and live in a tick infested area.
Can anyone tell me how to make a remedy for age spots or liver spots? I am sure there is a way not to spend thousands of dollars. Please help!
Hi Arax,
The articles below might be useful to you:
https://thelostherbs.com/use-this-plant-to-reverse-hyperpigmentation/
https://thelostherbs.com/diy-arnica-salve-for-age-spots/
Many blessings and good health!
Spraying Organic Apple Cider Vinegar helps a lot. Try it. I’ve found it helpful but even more so with skin tags & benign “mole” type growths that seem to appear with age.
Hi, Great article! Please could you post the citations to the research articles? I could use them for a paper in writing. Thank you!
Hi Bee,
Here it is: https://pubmed.ncbi.nlm.nih.gov/32154254/
Many blessings and good health!
How come you didn’t include Japanese Knotweed & Chinese Skullcap in your book ?
Hi Kate,
In The Lost Book of Herbal Remedies you can read about Skullcap (Scutellaria lateriflora) at page 132. Chinese skullcap (Scutellaria baicalensis) is native to East Asia, while American skullcap (Scutellaria lateriflora) is native to North America. However, many online health stores carry Chinese Skullcap tinctures, including Nicole’s Apothecary.
Japanese Knotweed is not a very common, or loved medicinal plant. It can damage foundations, sidewalks, and driveways by growing through cracks and crevices. It can also cause flooding by clogging storm drains and culverts. In addition, the plant produces a toxic substance that can contaminate water supplies and cause skin irritation. It is best to use a store-bought extract of this plant, like the one from Nicole’s Apothecary.
Many blessings and good health!
I was wondering if oregano or frankincense or clove would be good for tick borne illnesses? I have a tick borne illness along with dermatomyositis. I believe the tick illness has caused the DM. I am much better currently because of an antibiotic regiment.
Just wondering about these herbs being helpful for Lyme disease.
Thank you
Can you use all of these herbs together?